Why do you get Hyperreflexia in upper motor neuron lesions?
.
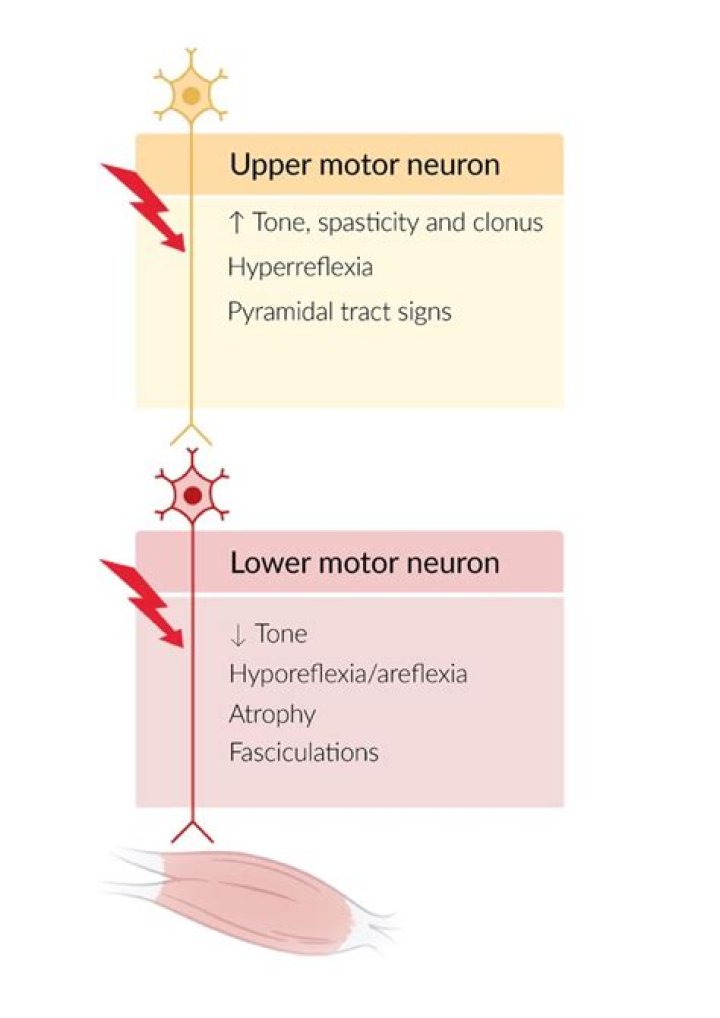
Keeping this in consideration, what are the signs of an upper motor neuron lesion?
Damage to upper motor neurons leads to a group of symptoms called upper motor neuron syndrome:
- Muscle weakness. The weakness can range from mild to severe.
- Overactive reflexes. Your muscles tense when they shouldn't.
- Tight muscles. The muscles become rigid and hard to move.
- Clonus.
- The Babinski response.
Subsequently, question is, why does spasticity occur in UMN lesions? Spasticity, a classical clinical manifestation of an upper motor neuron lesion, has been traditionally and physiologically defined as a velocity dependent increase in muscle tone caused by the increased excitability of the muscle stretch reflex.
Considering this, what does it mean if you have Hyperreflexia?
Hyperreflexia is defined as overactive or overresponsive reflexes. Examples of this can include twitching or spastic tendencies, which are indicative of upper motor neuron disease as well as the lessening or loss of control ordinarily exerted by higher brain centers of lower neural pathways (disinhibition).
What is Hoffman's sign?
Hoffman's sign or reflex is a test that doctors use to examine the reflexes of the upper extremities. This test is a quick, equipment-free way to test for the possible existence of spinal cord compression from a lesion on the spinal cord or another underlying nerve condition.
Related Question AnswersHow do you know you have motor neurone disease?
Symptoms of motor neurone disease (MND)- muscle aches, cramps, twitching.
- clumsiness, stumbling.
- weakness or changes in hands, arms, legs and voice.
- slurred speech, swallowing or chewing difficulty.
- fatigue.
- muscle wasting, weight loss.
Where are upper motor neuron cell bodies located?
The cell bodies of these neurons are located within the ventral horns of the spinal cord and within brainstem motor nuclei. Upper motor neurons, as defined clinically, are cortical neurons that innervate lower motor neurons (either directly or via local interneurons).Is Spinal Cord Injury upper or lower motor neuron?
Upper motor neuron signs may be present in limbs innervated by lower motor neurons caudal or inferior to the level of the spinal cord lesion. However, when the transection is due to severe, acute trauma, the setting of spinal or neurogenic shock may be initially present.What is upper motor neuron disease?
Upper motor neuron syndrome (UMNS) is the motor control changes that can occur in skeletal muscle after an upper motor neuron lesion. Following upper motor neuron lesions, affected muscles potentially have many features of altered performance including: weakness (decreased ability for the muscle to generate force)What is clonus a sign of?
Clonus is a series of involuntary, rhythmic, muscular contractions and relaxations. Clonus is a sign of certain neurological conditions, particularly associated with upper motor neuron lesions involving descending motor pathways, and in many cases is, accompanied by spasticity (another form of hyperexcitability).How can you tell the difference between UMN and LMN facial palsy?
To distinguish clinically between a LMN cause and UMN cause of the facial palsy, a patient with forehead sparing (i.e. no involvement to the occipitofrontalis muscle) will have a UMN origin to the palsy, due to the bilateral innervation of the forehead muscle).Is cerebellum upper motor neuron?
The cortical neuron is called the upper motor neuron. The first synapse is upon the lower motor neuron, whose cell body lives in the spinal cord. The second synapse is the neuromuscular junction itself. Lesions of the basal ganglia or cerebellum are neither upper nor lower motor neuron lesions.Is Hyperreflexia a sign of MS?
Hyperreflexia is a consequence of loss of inhibition from descending motor tracts. The Babinski's and Hoffmann's signs are special examples of loss of inhibition. Spasticity, which is a disorder of deep tendon reflex loops, is a companion of hyperreflexia.How do you know if you have Hyperreflexia?
The symptoms of AD may include:- anxiety and apprehension.
- irregular or racing heartbeat.
- nasal congestion.
- high blood pressure with systolic readings often over 200 mm Hg.
- a pounding headache.
- flushing of the skin.
- profuse sweating, particularly on the forehead.
- lightheadedness.