Why are Eskape pathogens important?
.
In this way, why are Eskape pathogens important in the clinic?
The ESKAPE pathogens are responsible for the majority of nosocomial infections and capable of 'escaping' the biocidal action of antimicrobial agents. The awareness of residential antimicrobial resistance can support selecting a convenient empirical therapeutic diet in diseases due to ESKAPE pathogens.
Also Know, who list of priority pathogens? 3 groups with different priorities This critical category includes Acinetobacter baumannii and Pseudomonas aeruginosa, both of which can cause wound infections, and the group of Enterobacteriaceae. Enterobacteria include Klebsiella, E. coli, Serratia and Proteus.
Similarly, you may ask, what does Eskape stand for?
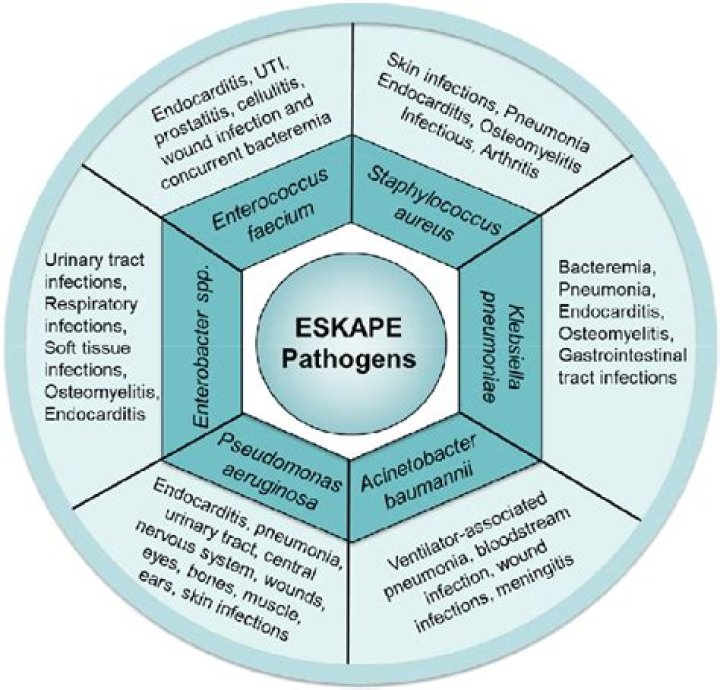
ESKAPE is an acronym encompassing the names of six bacterial pathogens commonly associated with antimicrobial resistance: ESKAPE is an acronym for their names and a reference to their ability to escape the effects of commonly used antibiotics through evolutionarily developed mechanisms.: Enterococcus faecium.
What are Eskape safe relatives?
ESKAPE pathogens are a class of bacteria that have formed multi-drug resistance and are major threats to human health in hospital settings. The ESKAPE pathogens some of the safe relatives are related to are Enterococcus faecium and Staphylococcus aureus.
Related Question AnswersWhat are the Eskape pathogens?
The term “ESKAPE” encompasses six such pathogens with growing multidrug resistance and virulence: Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, and Enterobacter spp. (Rice, 2008).What are nosocomial infections?
Nosocomial infections are infections that have been caught in a hospital and are potentially caused by organisms that are resistant to antibiotics. Methicillin-resistant Staphylococcus aureus (MRSA) is a type of staph bacteria that is resistant to certain antibiotics and may be acquired during hospitalization.What is the difference between broad spectrum and narrow spectrum antibiotics?
Narrow-spectrum antibiotics are only effective against a narrow range of bacteria, whereas broad-spectrum antibiotics are effective against a broad range of bacteria.How do you get antibiotic resistance?
A: Antibiotic resistance occurs when bacteria develop the ability to defeat the drugs designed to kill them. When bacteria become resistant, antibiotics cannot fight them, and the bacteria multiply.What is quorum sensing in bacteria?
Quorum sensing is the regulation of gene expression in response to fluctuations in cell-population density. Quorum sensing bacteria produce and release chemical signal molecules called autoinducers that increase in concentration as a function of cell density.What is Enterobacter species?
Enterobacter species are motile aerobic gram negative bacilli belonging to the family Enterobacteriaceae.Is Enterobacter the same as Enterobacteriaceae?
Enterobacter, (genus Enterobacter), any of a group of rod-shaped bacteria of the family Enterobacteriaceae. Enterobacter are gram-negative bacteria that are classified as facultative anaerobes, which means that they are able to thrive in both aerobic and anaerobic environments.Where is Acinetobacter found?
Acinetobacter [asz−in−ée−toe–back−ter] is a group of bacteria commonly found in soil and water. While there are many types or “species” of Acinetobacter and all can cause human disease, Acinetobacter baumannii [asz−in−ée−toe–back−ter boe-maa-nee-ie] accounts for about 80% of reported infections.What is the most dangerous bacteria in the world?
Here are some of the most dangerous.- Klebsiella pneumoniae. Approximately 3-5% of the population carry Klebsiella pneumoniae.
- Candida auris.
- Pseudomonas aeruginosa.
- Neisseria gonorrhea.
- Salmonellae.
- Acinetobacter baumannii.
- Drug resistant tuberculosis.
What antibiotics are used for bacteria?
The quinolones can be used for difficult-to-treat urinary tract infections when other options are aren't effective, hospital-acquired pneumonia, bacterial prostatitis, and even anthrax or plague.4. Quinolones.
| Generic | Brand Name Examples |
|---|---|
| ciprofloxacin | Cipro, Cipro XR |
| levofloxacin | Levaquin |
| moxifloxacin | Avelox |
What are priority diseases?
The first list of prioritized diseases was released in December 2015. Ebola virus disease and Marburg virus disease. Lassa fever. Middle East respiratory syndrome coronavirus (MERS-CoV) and Severe Acute Respiratory Syndrome (SARS) Nipah and henipaviral diseases.How do carbapenems work?
Closely related to penicillins, carbapenems are bactericidal beta-lactam antibiotics that bind to penicillin-binding proteins (PBPs). By binding and inactivating these proteins, carbapenems inhibit the synthesis of the bacterial cell wall, which leads to cell death.What is the name of the antibiotic?
This is why different antibiotics are used to treat different types of infection. The main types of antibiotics include: Penicillins - for example, phenoxymethylpenicillin, flucloxacillin and amoxicillin. Cephalosporins - for example, cefaclor, cefadroxil and cefalexin.Do we need new antibiotics?
Today, drug-resistant infections are a serious threat to people's health. Hundreds of thousands of lives are lost every year because of infections that can no longer be treated with existing drugs. Discovering new antibiotics, able to kill drug-resistant bacteria, is essential to saving modern medicine.What are infectious diseases?
Infectious diseases affect billions of people around the globe annually. According to WHO and the CDC, these infectious diseases are the five most common.- Hepatitis B.
- Malaria.
- Hepatitis C.
- Dengue.
- Tuberculosis.
What are two causes of multidrug resistant organisms?
Common multidrug-resistant organisms are usually bacteria:- Vancomycin-Resistant Enterococci (VRE)
- Methicillin-Resistant Staphylococcus aureus (MRSA)
- Extended-spectrum β-lactamase (ESBLs) producing Gram-negative bacteria.
- Klebsiella pneumoniae carbapenemase (KPC) producing Gram-negatives.



