How often are hedis measures revised
Measures are revised every year to include newer and even more effective Best Practice Guidelines. According to a 2005 study, HEDIS-Medicaid 3.0 measures covered only 22% of the services recommended by the second U.S. Preventive Services Task Force (USPSTF).
How often are HEDIS measures revised quizlet?
Plans not obtaining 4 Stars or better may be penalized. How often are HEDIS measures revised? Measures are added, deleted, and revised annually.
Will there be a HEDIS 2021?
The transition will coincide with the HEDIS Timeline transition process starting in HEDIS 2020 and completing in 2021.
How often is HEDIS measured?
Measures for HEDIS, which are revised every year, are strictly defined, as are the reporting guidelines. Here are 10 facts about HEDIS reporting.How many HEDIS measures are there for 2021?
HEDIS MY 2020 & MY 2021 Digital Measures for Traditional Reporting (8 Digital Measures)
What is the goal of HEDIS?
HEDIS is a comprehensive set of standardized performance measures designed to provide purchasers and consumers with the information they need for reliable comparison of health plan performance. HEDIS Measures relate to many significant public health issues, such as cancer, heart disease, smoking, asthma, and diabetes.
Who developed and maintains HEDIS?
NCQA develops and maintains a standardized set of quality measures called “HEDIS®” that many states use for these efforts.
What are 2 types of HEDIS measures?
The tables below explain the National Committee for Quality Assurance (NCQA) Healthcare Effectiveness Data and Information Set (HEDIS) measures for two types of care: preventive health care (children and adolescents, women and adolescent girls, adults, and seniors) and condition-specific care.What is a good HEDIS score?
For those in the eye care industry, receiving excellent HEDIS scores can be financially beneficial, while also improving the quality of care. CMS uses a 5-‐star system to rate Health Plans, with 1 star being “poor” and 5 stars being “excellent.” Bonuses for high star ratings range from 1.5 percent to 5 percent.
How long is HEDIS season?HEDIS Abstraction job postings start going up in early Fall, around mid-September with the peak time being October-November. Interviews are typically conducted in November-December with hiring decisions made by December-January for start dates of January-February.
Article first time published onIs HEDIS only for Medicare?
All Medicare plans required by CMS to submit HEDIS are included in the published ratings. Medicare plans that are not required by CMS to submit HEDIS are not included in the published ratings unless they have earned NCQA Accreditation.
How can I improve my HEDIS score?
Some HEDIS and CMS Star Ratings measures are based on measures across six domains of care including effectiveness of care and utilization. One of the ways to improve your scores is through increased outreach and better follow-up patient care.
What are the CMS star ratings?
Star Ratings are released annually and reflect the experiences of people enrolled in Medicare Advantage and Part D prescription drug plans. The Star Ratings system supports CMS’s efforts to empower people to make health care decisions that are best for them.
How do I get HEDIS training?
- Request an Application. Submit an inquiry through My NCQA. …
- Review Handbook and Application. …
- Submit Your Application. …
- NCQA Approves Your Application. …
- Learn Requirements and Audit Process. …
- Sit for Your Exam.
How do you close HEDIS gaps?
- Amplify every connection. To improve quality measure performance, every patient or plan member connection must address more than one objective. …
- Teach at every touchpoint. …
- Coordinate care as needed.
How is the Healthcare Effectiveness Data and Information Set HEDIS used?
The Healthcare Effectiveness Data and Information Set (HEDIS) is a tool used by more than 90 percent of U.S. health plans to measure performance on important dimensions of care and service. … Persons enrolled in health plans that report quality results using HEDIS.
How often is NCQA certification?
Accredited-2 years: NCQA awards a status of Accredited – 2 years to organizations that demonstrate performance of the functions outlined in the standards for CM accreditation. Denied: NCQA denies Accreditation to organizations that did not meet NCQA requirements during the Accreditation Survey.
What does a HEDIS nurse do?
What do HEDIS nurses do? They collect and review data from patient charts and other medical records from hospitals, doctors’ offices and various health care providers to measure and help improve quality.
Who owns NCQA?
Our 12-person Leadership Team includes our founder, Margaret E. O’Kane. She started NCQA almost 30 years ago, working by herself in a borrowed office.
What are HEDIS care gaps?
Care Gaps identify missing recommended preventive care services so that you may address them when your patient comes in for an office visit. Care Gaps are based on HEDIS measures and may impact your quality scores.
How many HEDIS measures are there?
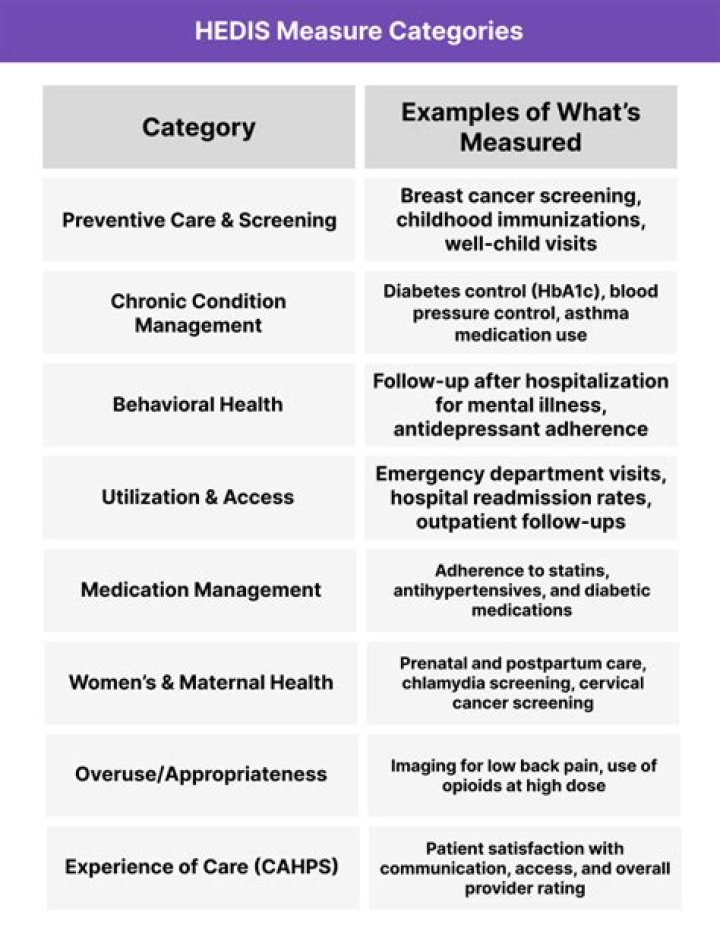
HEDIS consists of 71 measures across 8 domains of care. Because so many plans use HEDIS and because the measures are so specifically defined, HEDIS can be used to make comparisons among plans.
What data does HEDIS require?
- Effectiveness of Care.
- Access/Availability of Care.
- Experience of Care.
- Utilization and Risk Adjusted Utilization.
- Health Plan Descriptive Information.
- Measures Reported Using Electronic Clinical Data Systems.
How is HEDIS used in healthcare?
HEDIS (pronounced he´-dus) stands for Healthcare Effectiveness Data and Information Set. Employers and individuals use HEDIS to measure the quality of health plans. HEDIS measures how well health plans give service and care to their members.
What is HEDIS medical record review?
A HEDIS chart review is when the National Committee for Quality Assurance (NCQA) reviews a patient’s medical records to determine if the quality of care measures have been met. Medical chart reviews are also the data source used by the NCQA to determine any incentives or financial rewards for health plans.
What percentage of health plans use HEDIS?
More than 90 percent of health plans—HMOs, POS plans, and PPOs—use HEDIS to measure performance.
Who is required to report HEDIS measures?
All plans must report HEDIS/ CAHPS for the HEDIS reporting date after their first full year of Accreditation. Plans with fewer than 15,000 members are not required to report. All plans must report HEDIS/ CAHPS for the HEDIS reporting date in their third year of Accreditation.
Do HEDIS nurses work year round?
HEDIS efforts continue year-round, but the actual abstraction process only lasts 4-5 months per year and this is the primary role you will find on job boards.
How do I become a HEDIS nurse abstractor?
The qualifications that you need to become a remote HEDIS nurse include a nursing degree, knowledge of auditing procedures and HEDIS measurement variables, and computer skills to access medical records. You start your nursing career by earning an associate or bachelor’s degree in nursing.
How much do HEDIS nurses make?
The average salary for a hedis nurse is $33.78 per hour in the United States.
How are HEDIS rates calculated?
How Are Rates Calculated? HEDIS rates can be calculated in two ways: administrative data or hybrid data. Administrative data consists of claim or encounter data submitted to the health plan. Hybrid data consists of both administrative data and a sample of medical record data.
What is HEDIS star rating?
For HEDIS measures, Star Ratings use a clustering algorithm that identifies “gaps” in the data and creates five categories (one for each Star Rating). Star Ratings incorporate a measure on improvement into plans’ overall score, with a weight of 5. HPR does not incorporate an improvement bonus.