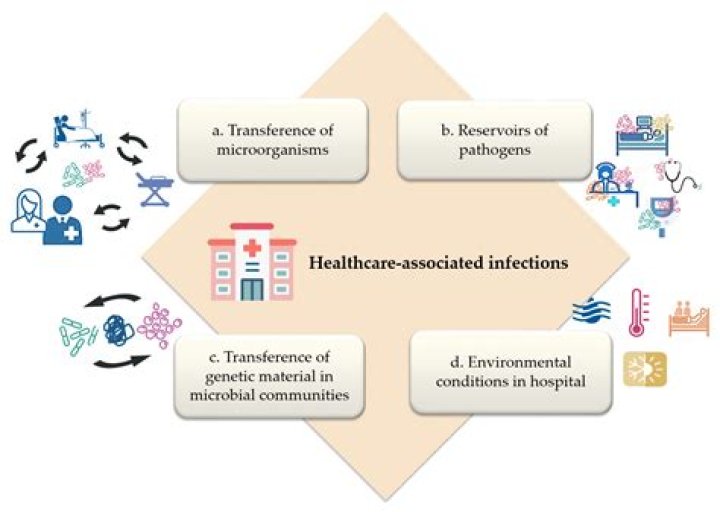
During hospitalization, patient is exposed to pathogens through different sources environment, healthcare staff, and other infected patients. Nosocomial infections can be controlled by practicing infection control programs, keep check on antimicrobial use and its resistance, adopting antibiotic control policy..
Besides, how can nosocomial infections be prevented?
10 Steps to Preventing Spread of Infection in Hospitals
- Wash Your Hands. Hand washing should be the cornerstone of reducing HAIs.
- Create an Infection-Control Policy.
- Identify Contagions ASAP.
- Provide Infection Control Education.
- Use Gloves.
- Provide Isolation-Appropriate Personal Protective Equipment.
- Disinfect and Keep Surfaces Clean.
- Prevent Patients From Walking Barefoot.
Beside above, what is a specific example of a nosocomial infection? Key Points. Some well known nosocomial infections include: ventilator-associated pneumonia, Methicillin resistant Staphylococcus aureus, Candida albicans, Acinetobacter baumannii, Clostridium difficile, Tuberculosis, Urinary tract infection, Vancomycin-resistant Enterococcus and Legionnaires' disease.
Keeping this in view, how can hospital acquired infection be controlled?
Prevention and control - Remove sources of infection by treating infections and decontamination procedures; - Prevent transfer with good hand hygiene, aseptic procedures, and appropriate isolation; - Enhance resistance with good nutrition, and appropriate antibiotic prophylaxis or vaccination.
How are nosocomial infections transmitted?
Nosocomial infections are infections that develop as a result of a stay in hospital or are produced by microorganisms and viruses acquired during hospitalization. They may be endogenous, arising from an infectious agent present within a patient's body, or exogenous, transmitted from another source within the hospital.
Related Question Answers
What are the 3 methods of infection control?
Infection Control and Prevention - Standard Precautions - Standard Precautions.
- Hand Hygiene.
- Personal Protective Equipment (PPE)
- Needlestick and Sharps Injury Prevention.
- Cleaning and Disinfection.
- Respiratory Hygiene (Cough Etiquette)
- Waste Disposal.
- Safe Injection Practices.
How can infection control be improved?
Four infection prevention and process improvement experts weigh-in on the 10 best strategies for prevention of infections. - Hand Hygiene.
- Environmental hygiene.
- Screening and cohorting patients.
- Vaccinations.
- Surveillance.
- Antibiotic stewardship.
- Care coordination.
- Following the evidence.
How can we prevent cross infection in Ward?
Five Things You Can Do To Prevent Infection - Clean Your Hands. Use soap and warm water.
- Make sure health care providers clean their hands or wear gloves.
- Cover your mouth and nose.
- If you are sick, avoid close contact with others.
- Get shots to avoid disease and fight the spread of infection.
What are the five basic principles for infection control?
These include standard precautions (hand hygiene, PPE, injection safety, environmental cleaning, and respiratory hygiene/cough etiquette) and transmission-based precautions (contact, droplet, and airborne).How can we reduce Hais?
Infection control practices to reduce HAI include the use of protective barriers (e.g., gloves, gowns, face mask, protective eyewear, face shield) to reduce occupational transmission of organisms from the patient to the health care worker and from the health care worker to the patient.How can the risk of healthcare associated infections be reduced?
How to Reduce the Risk of Health Care Associated Infections - Speak up! Ask your doctor about any questions or worries that you may have.
- Keep hands clean!
- Be smart about antibiotics.
- Know the signs and symptoms of an infection.
- Diarrhea can be a sign of certain types of infections.
- Protect yourself.
How do I start an infection control program?
8 Steps to Effective Hospital Infection Control Programs - Educate staff.
- Create a multidisciplinary team.
- Collect data.
- Analyze the data.
- Communicate the data.
- Develop action plans.
- Additional activities of the infection control department.
- Stay up-to-date on policies and news.
Who is responsible for infection control in hospital?
56: These doctors are generally microbiologists and/or infectious disease specialists who are responsible for a range of services in the hospital, including infection control. We refer to them as “infection control doctors”, but infection control is only one of a number of activities in which they are involved.What is the goal of infection control?
The mission of the WHO Infection Prevention and Control in Health Care initiative is to assist Member States in reducing dissemination of infections associated with healthcare, by assisting with the assessment, planning, implementation and evaluation of national infection control policies.What do you call a hospital acquired infection?
A hospital-acquired infection (HAI), also known as a nosocomial infection, is an infection that is acquired in a hospital or other health care facility. To emphasize both hospital and nonhospital settings, it is sometimes instead called a health care–associated infection (HAI or HCAI).What is infection control in hospitals?
Infection control is the discipline concerned with preventing nosocomial or healthcare-associated infection, a practical (rather than academic) sub-discipline of epidemiology. It is an essential, though often underrecognized and undersupported, part of the infrastructure of health care.What bacteria causes nosocomial infection?
Bacteria are the most common pathogens responsible for nosocomial infections. Some belong to natural flora of the patient and cause infection only when the immune system of the patient becomes prone to infections. Acinetobacter is the genre of pathogenic bacteria responsible for infections occurring in ICUs.Why is infection control important in hospitals?
Why is infection prevention and control so important in a hospital environment? Healthcare-acquired infections are one of the most common complications of health care. A well-functioning Infection Prevention and Control program helps minimize these risks for our patients, residents, visitors and our staff.What is the chain of infection?
The chain of infection, if we think of it as an actual chain, is made up of six different links: pathogen (infectious agent), reservoir, portal of exit, means of transmission, portal of entry, and the new host. Each link has a unique role in the chain, and each can be interrupted, or broken, through various means.What is the most common type of nosocomial infection?
According to the CDC, the most common pathogens that cause nosocomial infections are Staphylococcus aureus, Pseudomonas aeruginosa, and E. coli. Some of the common nosocomial infections are urinary tract infections, respiratory pneumonia, surgical site wound infections, bacteremia, gastrointestinal and skin infections.Is MRSA a nosocomial infection?
Methicillin-resistant Staphylococcus aureus (MRSA) is a major nosocomial pathogen worldwide. Patients infected with MRSA tended to have more co-morbidities, longer lengths of stay (LOS) and greater exposure to antibiotics than MSSA-infected patients.Is E coli nosocomial?
E. coli is the most common cause of hospital-acquired urinary tract infections. Research indicates that nosocomial UTI-causing E. coli strains differ from community-acquired strains in their virulence traits.What is an example of an endogenous infection?
Endogenous Bacteria. Disease can occur when microbes included in normal bacteria flora enter a sterile area of the body such as the brain or muscle. This is considered an endogenous infection. A prime example of this is when the residential bacterium E. coli of the GI tract enters the urinary tract.What are five things that increase the risk of nosocomial infection?
Certain underlying diseases, procedures, hospital services, and categories of age, sex, race, and urgency of admission were all found to be significant risk factors for nosocomial infection.